Analysis of Racial/Ethnic Representation in Select Basic and Applied Cancer Research Studies
Abstract
Over the past decades, consistent studies have shown that race/ethnicity have a great impact on cancer incidence, survival, drug response, molecular pathways and epigenetics. Despite the influence of race/ethnicity in cancer outcomes and its impact in health care quality, a comprehensive understanding of racial/ethnic inclusion in oncological research has never been addressed. We therefore explored the racial/ethnic composition of samples/individuals included in fundamental (patient-derived oncological models, biobanks and genomics) and applied cancer research studies (clinical trials).
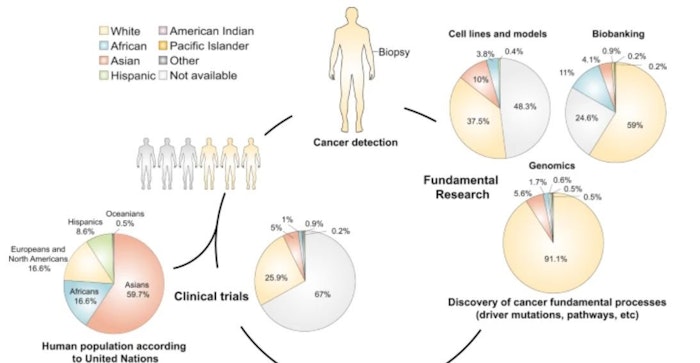
Regarding patient-derived oncological models (n = 794), 48.3% have no records on their donor’s race/ethnicity, the rest were isolated from White (37.5%), Asian (10%), African American (3.8%) and Hispanic (0.4%) donors. Biobanks (n = 8,293) hold specimens from unknown (24.56%), White (59.03%), African American (11.05%), Asian (4.12%) and other individuals (1.24%). Genomic projects (n = 6,765,447) include samples from unknown (0.6%), White (91.1%), Asian (5.6%), African American (1.7%), Hispanic (0.5%) and other populations (0.5%). Concerning clinical trials (n = 89,212), no racial/ethnic registries were found in 66.95% of participants, and records were mainly obtained from Whites (25.94%), Asians (4.97%), African Americans (1.08%), Hispanics (0.16%) and other minorities (0.9%). Thus, two tendencies were observed across oncological studies: lack of racial/ethnic information and overrepresentation of Caucasian/White samples/individuals. These results clearly indicate a need to diversify oncological studies to other populations along with novel strategies to enhanced race/ethnicity data recording and reporting.