Harmonization of Postmortem Donations for Pediatric Brain Tumors and Molecular Characterization of Diffuse Midline Gliomas
Abstract
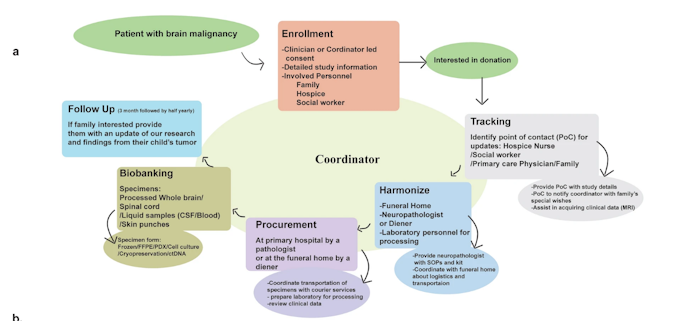
Children diagnosed with brain tumors have the lowest overall survival of all pediatric cancers. Recent molecular studies have resulted in the discovery of recurrent driver mutations in many pediatric brain tumors. However, despite these molecular advances, the clinical outcomes of high grade tumors, including H3K27M diffuse midline glioma (H3K27M DMG), remain poor. To address the paucity of tissue for biological studies, we have established a comprehensive protocol for the coordination and processing of donated specimens at postmortem. Since 2010, 60 postmortem pediatric brain tumor donations from 26 institutions were coordinated and collected. Patient derived xenograft models and cell cultures were successfully created (76% and 44% of attempts respectively), irrespective of postmortem processing time. Histological analysis of mid-sagittal whole brain sections revealed evidence of treatment response, immune cell infiltration and the migratory path of infiltrating H3K27M DMG cells into other midline structures and cerebral lobes. Sequencing of primary and disseminated tumors confirmed the presence of oncogenic driver mutations and their obligate partners. Our findings highlight the importance of postmortem tissue donations as an invaluable resource to accelerate research, potentially leading to improved outcomes for children with aggressive brain tumors.
Acknowledgements
Authors would like to acknowledge patients and their families for generous donation of tumor tissue for our study. We would like to thank all the pathologists who have helped us with the procurement. We are grateful for funding from Gift from a Child Initiative, Swifty Foundation, Smashing Walnuts Foundation, Piedmont Community, The Gabriella Miller Kids First Data Resource Center, Goldwin Foundation, Pediatric Brain Tumor Foundation, Zickler Family Foundation, Isabella Kerr Molina Foundation, The Lilabean Foundation for Pediatric Brain Cancer Research, Matthew Larson Foundation, Children Brain Tumor Foundation