Developing a Novel Tumor Model to Screen for New Therapies for Spinal Ependymoma
Email Principal Investigator

Linda M. Smith-Resar
CBTN Specimen
CBTN Participants
CBTN Pre-clinical Models
Backer
Alex's Lemonade Stand Foundation
About this
Project
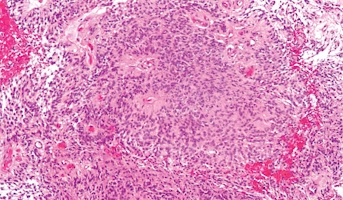
Spinal ependymomas (SEs) are rare tumors of the central nervous system that currently have limited treatment options and poor outcomes for advanced cases. Unfortunately, SEs do not respond well to radiation therapy or chemotherapy and almost half of patients will experience tumor recurrence. Because these tumors are rare, there are few tumor models and limited research to define underlying drivers and targets for therapy. To address this significant gap, this project proposes to develop an innovative tumor model based on recent discoveries. Previous research has found that primary tumor cells derived from the ectoderm (the spinal cord, periphery nerves, and brain) can be cultured indefinitely using special methods. These “conditionally reprogrammed cells” (CRCs) form spheres in vitro and replicate tumor pathology, allowing for their use in models used to predict drug response. The goals of this project are to generate CRCs from primary tumors or normal developing spinal cord. This will be possible due to cell lines provided by the Children’s Brain Tumor Network. Researchers will begin to screen a unique library of drugs already approved for use in humans for agents that selectively kill CRCs from tumors, but not normal tissue. This work could provide new avenues for personalized therapy for children with spinal ependymomas, and possibly other tumors of ectodermal origins. If successful, researchers will translate their approach to the clinics to improve outcomes for children with high grade spinal ependymoma.
Ask The
Scientists
What are the goals of this project?
The goals of this project are to generate conditional reprogrammed cells that can be used as models of spinal ependymoma to predict tumor response to various drugs and perform drug screens to learn more about therapeutic opportunities.
What is the impact of this project?
Current models are insufficient for the study of spinal ependymoma, but this project will explore new discoveries in the hopes of developing models whose use will improve outcomes for pediatric spinal ependymoma patients. Moreover drugs will be screened on the cell line to identify available therapeutic options.
Why is the CBTN request important to this project?
The work being done in this project would not be possible without rare specimens provided by the Children’s Brain Tumor Network.
Specimen Data
The Children's Brain Tumor Network contributed to this project by providing cell lines.
Meet The
Team
Drs. Li Luo and Lingling Xian