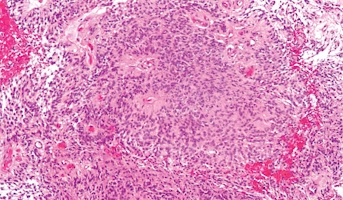
Molecular and Functional Characterization of Childhood Supratentorial Ependymoma
Email Principal Investigator

Vijay Ramaswamy
CBTN Data
CBTN Specimen
CBTN Participants
Backer
Canadian Institutes for Health Research Project Grant
Institutional Funds
About this
Project
Ependymoma is a common brain tumor of childhood and can occur anywhere in the nervous system. Although classically described as a single entity, recent research has made it very clear that different areas of ependymoma are totally different diseases. Specifically, these areas are the supratentorial, posterior fossa and spinal compartments. Previous classification has shown that supratentorial ependymoma comprises 3 distinct subgroups, ST-EPN-RELA, ST-EPN-YAP1 and ST-EPN-SE (subependymoma). ST-EPN-RELA has a very poor prognosis and ST-EPN-YAP1 comprises infants with a very good prognosis. However, the vast majority of supratentorial ependymoma are ST-EPN-RELA, and within ST-EPN-RELA there is a wide range of clinical differences leading to a gap in personalized care options. Currently, it is unclear which patients are predicted to do well within this group, and whether there exists established differences that can help guide clinical care. Current therapies include surgery and radiation, but further research such as this project could open new opportunities for therapy and guide the prioritization of clinical trials. The Children's Brain Tumor Network contributed to this project by providing hard-to-acquire tumor DNA, tumor RNA and access to data from the Pediatric Brain Tumor Atlas.
Ask The
Scientists
What are the goals of this project?
Researchers will explore the differences between distinct subgroups of ependymoma in an effort to establish personalized therapeutics.
What is the impact of this project?
A greater understanding of ependymoma subtypes will help guide clinical care of pediatric patients, hopefully leading to better outcomes.
Why is the CBTN request important to this project?
The specimens and data necessary to complete this data are rare, making access to such samples and the Pediatric Brain Tumor Atlas necessary to this project.
Specimen Data
The Children's Brain Tumor Network contributed to this project by providing tumor DNA, tumor RNA and access to the Pediatric Brain Tumor Atlas.
Meet The