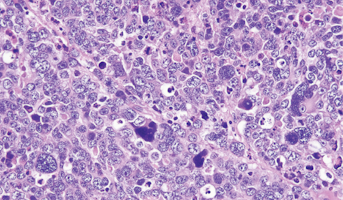
Determining Prognostic Factors and Genetic Markers that Impact Survival in Recurrent Pediatric Medulloblastoma
Email Principal Investigator

Chetan Bettegowda
CBTN Data
Backer
Johns Hopkins University School of Medicine Dean's Funding Grant
About this
Project
Medulloblastoma is the most common malignant brain tumor in children and is classified as a grade IV tumor. Previous research has identified four different subgroups of medulloblastomas— wingless (WNT), sonic hedgehog (SHH), Group 3, and Group 4. Today, medulloblastoma in the pediatric population has an overall 70% survival rate at five years from diagnosis but survival rates vary across subtypes. In about 20% of cases, medulloblastoma reoccurs and is very often a fatal event. This project will analyze data about patients and tumors to determine what impacts survival for patients with recurrent medulloblastoma. Guidelines for treatment of relapsed medulloblastoma have not been established due to the broad variety of medulloblastoma treatments that exist. In addition, recent evidence has been found that recurrent medulloblastoma tumors share only 12% of genetic mutations found in patient’s first tumor. This genetic difference suggests that recurrent tumors might be best treated with different targeted therapies than those used at the onset of the disease. Researchers will use data that includes demographic, genetic subtype and other tumor characteristics, treatment modality, and genetic data from the Pediatric Brain Tumor Atlas. Through interrogation of all of this information, it will be possible for researchers to study what factors impact overall and progression-free survival after the recurrence of medulloblastoma in the pediatric population by tumor subtype, paving the way for the development of personalized therapies.
Ask The
Scientists
What are the goals of this project?
This project will analyze patient and tumor factors to determine what impacts survival in this patient population.
What is the impact of this project?
The recurrence of medulloblastoma, which occurs in approximately 20% of cases, is considered an almost completely fatal event; survival rates at 3 years have been reported at a mere 18%. Further, guidelines for treatment of relapsed medulloblastoma have not been established due to the heterogeneity of treatment that exists.In addition, recent evidence that recurrent medulloblastoma tumors share only 12% of genetic mutations found in the dominant clonal tumor cell at initial diagnosis suggests that recurrent tumors might be best treated with different targeted therapies than those used at the onset of the disease.
Why is the CBTN request important to this project?
Using data that includes demographic, genetic subtype and other tumor characteristics, treatment modality, and whole-genome sequencing information from the Children’s Brain Tumor Network (CBTN) databank, it will be possible to study the factors that impact overall and progression-free survival after the recurrence of medulloblastoma in the pediatric population by tumor subtype.
Specimen Data
The Children's Brain Tumor Network contributed to this project by providing access to the Pediatric Brain Tumor Atlas.