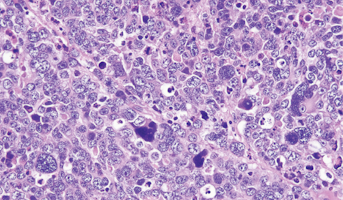
Released Tumor DNA in the CSF for the Diagnosis and Monitoring of Pediatric Brain Tumors
Email Principal Investigator

Chetan Bettegowda
CBTN Specimen
CBTN Participants
CBTN Samples
Backer
Alex's Lemonade Stand Foundation
NCI U01CA230691-01
NCI CA230400-01
About this
Project
Through the use of CT and MRI, clinicians use anatomical features to assess the state of disease in patients with cancer. Unfortunately, these video methods do not quantify the level of disease or differentiate true areas of cancer from treatment related changes. One of the challenges is the lack of robust biomarkers that can be used to monitor diseases. Biomarkers are measurable indicators of disease state and can be used for prognosis purposes. Identification of biomarkers could greatly aid clinicians in diagnosis, prognosis, and treatment of pediatric brain tumors. Identifying means for testing that do not require tumor tissue would reduce the risk of permanent neurological deficit for patients with tumors that are particularly challenging to remove. One line of investigation that researchers on this project have been pursuing is the detection of cell free DNA shed from tumor cells into body fluids such as plasma and cerebrospinal fluid (CSF). All cells, including tumor cells and non-malignant cells, shed DNA, called cell-free DNA (cfDNA), into the circulatory system. Researchers recently demonstrated that levels of tumor derived DNA are significantly enriched in the CSF of individuals with brain tumors, including medulloblastoma. CSF has the potential to act as a “liquid biopsy” for children with brain tumors. Potential applications of this sort of detection include assessment of disease burden, drug resistance, and tumor evolution. Researchers have successfully completed this work for other tumor types, and will use 5 CSF samples provided by the Children’s Brain Tumor Network to extend this work to pediatric medulloblastoma.
Ask The
Scientists
What are the goals of this project?
Researchers will explore the usefulness of CSF samples as liquid biopsy for the diagnosis and prognosis of pediatric medulloblastoma.
What is the impact of this project?
If validated as a successful option, liquid biopsy using CSF would be a new, minimally invasive diagnostic option for patients with medulloblastoma.
Why is the CBTN request important to this project?
Researchers have carried out similar work for other tumor types and will be able to extend this work to medulloblastoma using rare samples provided by the Children’s Brain Tumor Network.
Specimen Data
The Children's Brain Tumor Network contributed to this project by providing 5 cerebral spinal fluid samples for a pilot cohort.