Elucidating Heterogeneity of Resistance Across Molecular Subgroups of Pediatric Ependymomas to Inform Future Therapeutics

Jeffrey Greenfield
CBTN Specimen
CBTN Participants
CBTN Pre-clinical Models
Backer
Internal funding
About this
Project
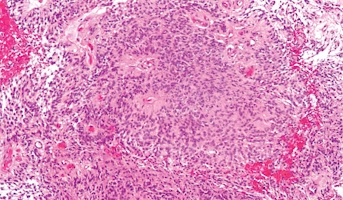
Intracranial ependymomas are a common pediatric brain cancer. Advances in molecular profiling over the past decade have led to the identification of nine distinct molecular subgroups of ependymomas across three anatomical areas of the central nervous system. Radiation therapy, though effective at killing tumor cells, can cause major toxicities for patients and lead to the potential development of systemic resistance to subsequent therapies. It is still important to determine which molecular subgroups of ependymomas may benefit from post-radiation chemotherapy and which patients are resistant to post-radiation treatment. The central hypothesis of this research is that molecular subgroups of ependymomas acquire identifiable mutations following ionizing radiation exposure. Researchers believe this in turn contributes to the development of resistance to treatment. Researchers expect that the completion of this project will help elucidate the difference in response to radiation and chemotherapy across molecular ependymoma subgroups, informing future therapeutics. This project will involve the study of cell lines from each of the subgroups most common in children, specifically PF-EPN-A, STEPN- RELA, ST-EPN-YAP1. Ependymoma tumors are rare in children and ependymoma cell lines are difficult to establish, making the Children’s Brain Tumor Network provision of preclinical models particularly important to this work.
Ask The
Scientists
What are the goals of this project?
Researchers will analyze cell lines from many subgroups of ependymoma in an effort to understand why some subgroups are more resistant to treatment than others.
What is the impact of this project?
Researchers expect that the completion of this project will help in understanding the difference in response to radiation and chemotherapy across molecular ependymoma subgroups, informing future therapeutics.
Why is the CBTN request important to this project?
Ependymoma cell lines are hard to establish, making the Children’s Brain Tumor Network’s provision of high quality cell lines integral to this work.
Specimen Data
The Children's Brain Tumor Network is contributing to this project by providing preclinical models.
Meet The
Team

New York, NY, USA

New York, NY, USA

New York, NY, USA

New York, NY, USA

New York, NY, USA