Jeffrey Greenfield

About
Vice Chairman for Academic Affairs and Associate Residency Director; Associate Professor of Neurological Surgery and Pediatrics, Department of Neurological Surgery
Weill Cornell Medicine Pediatric Brain & Spine Center
Dr. Greenfield’s directs multiple research projects pertaining to pediatric brain tumors, in particular, basic research examining the brain tumor microenvironment, tumor immunology, and precision medicine. This research has been externally funded and widely published and he has received national awards from neurosurgical societies. He has lectured internationally on these subjects and together with Dr. Mark Souweidane he co-directs the Children’s Brain Tumor Project, focusing on novel approaches and innovative care for children with rare and inoperable brain tumors.
Expertise
Neurosurgery

Weill Cornell Medicine
scientific
Projects
Specimen
Ongoing
Epigenetic Basis of Gender Differences in Pediatric GBM
CBTN specimen will be used for reduced representation bisulfite sequencing - we will be profiling the transcriptome and epigenome. We will then compare these profiles between boys and girls with pediatric GBM to identify lesions that cause the difference in clinical outcomes of these patients.
HGG

Sheng Li

Data
Ongoing
Searching for Differences in Molecular Profile of Pediatric Gliomas
Understanding the similarities and differences across subtypes of glioma is necessary to provide targeted care. Researchers will utilize data from the Pediatric Brain Tumor Atlas in an effort to more accurately categorize and treat pediatric high grade gliomas.
HGG, DIPG

Nikolay Ivanov
Data
Ongoing
Relationships Between Genomic, Imaging, and Histopathologic Characteristics in Pediatric Brain Tumors
Genomic data, tumor imagery, and text-based data are all important in the diagnosis and treatment of cancers. Through computational comparisons of these data types made available through the Pediatric Brain Tumor Atlas, researchers seek to improve the accuracy of cancer diagnostics.
All Brain Tumor Types

Specimen
Ongoing
Elucidating Heterogeneity of Resistance Across Molecular Subgroups of Pediatric Ependymomas to Inform Future Therapeutics
Intracranial ependymomas are a common pediatric brain cancer with many subgroups that may respond differently to different therapies. Using cell lines provided by the Children’s Brain Tumor Network, researchers seek to better understand these differences in an effort to advance positive patient outcomes.
Ependymoma

Jeffrey Greenfield

Data
Ongoing
Spatial Evolution and Somatic Mutations Spectrum of Gliomatosis Cerebri
The development of treatment for Gliomatosis cerebri and other high grade gliomas relies on a comprehensive understanding of each tumor type. Using the Pediatric Brain Tumor Atlas alongside other open access datasets, researchers will map and analyze how tumors change over time, across locations, and the specific proteins created in Gliomatosis cerebri.
Ependymoma, DIPG

Jeffrey Greenfield
research
Interests
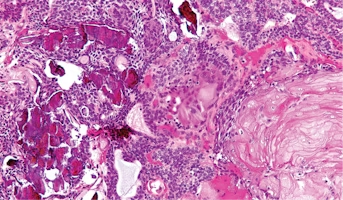
Craniopharyngioma
Childhood craniopharyngiomas are rare tumors usually found near the pituitary gland (a pea-sized organ at the bottom of the brain that controls other glands) and the hypothalamus (a small cone-shaped organ connected to the pituitary gland by nerves).Craniopharyngiomas are usually part solid mass and
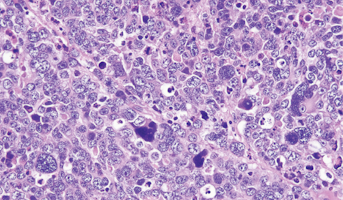
Medulloblastoma
Medulloblastomas comprises the vast majority of pediatric embryonal tumors and by definition arise in the posterior fossa, where they constitute approximately 40% of all posterior fossa tumors. Other forms of embryonal tumors each make up 2% or less of all childhood brain tumors.The clinical feature
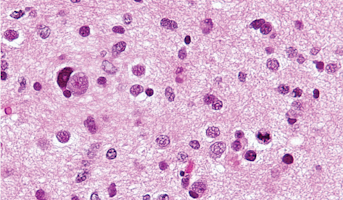
High-Grade Glioma
High-grade Gliomas (HGG) or astrocytomas in children nearly always result in a dismal prognosis. Although novel therapeutic approaches are currently in development, preclinical testing has been limited, due to a lack of pediatric-specific HGG preclinical models. These models are needed to help test
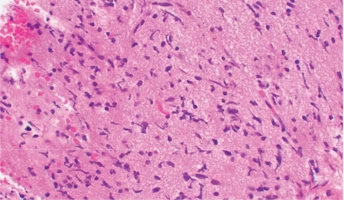
Diffuse Intrinsic Pontine Glioma
A presumptive diagnosis of DIPG based on classic imaging features, in the absence of a histologic diagnosis, has been routinely employed. Increasingly however, histologic confirmation is obtained for both entry into research studies and molecular characterization of the tumor.[5] New approaches with