

Nikolay Ivanov
CBTN Data
Backer
TL1 Grant (Award Number TL1TR002386)
About this
Project
Glioma is a type of brain cancer in which glial cells, a specific type of cell in the brain, become cancerous. In this study, researchers will examine how the DNA in glioma cells varies between different groups of patients and how these differences in DNA affect gene expression. This will allow for a greater understanding of how pediatric glioma develops, how it differs between patients, and how childhood glioma differs from adult glioma. To complete this research, RNA sequencing data from pediatric high grade gliomas (pHGGs) will be used to examine glioma gene expression. Particularly, researchers are searching for previously uncharacterized subtypes of pHGG. Understanding the similarities and differences of these subtypes could lead to more accurate diagnosis and more effective cancer therapies. Data from the Pediatric Brain Tumor Atlas, specifically the RNA sequencing data from pHGG samples, will be integral to the characterization of pHGG in this study.
Ask The
Scientists
What are the goals of this project?
Researchers will seek greater understanding of how pediatric glioma develops, how it differs between patients, and how childhood glioma differs from adult glioma.
What is the impact of this project?
Understanding the mechanisms across subtypes of pediatric high grade glioma could lead to more accurate diagnostics and treatments.
Why is the CBTN request important to this project?
Researchers need RNA sequencing data from rare pHGG samples to complete this work, and the Pediatric Brain Tumor Atlas provides this data across many subtypes.
Meet The
Team
related
Histologies
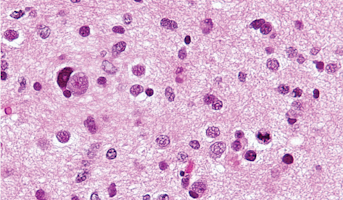
High-Grade Glioma
High-grade Gliomas (HGG) or astrocytomas in children nearly always result in a dismal prognosis. Although novel therapeutic approaches are currently in development, preclinical testing has been limited, due to a lack of pediatric-specific HGG preclinical models. These models are needed to help test
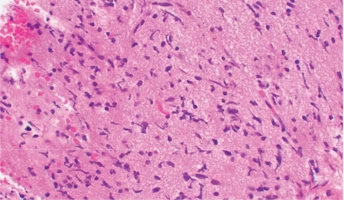
Diffuse Intrinsic Pontine Glioma
A presumptive diagnosis of DIPG based on classic imaging features, in the absence of a histologic diagnosis, has been routinely employed. Increasingly however, histologic confirmation is obtained for both entry into research studies and molecular characterization of the tumor.[5] New approaches with





