Health Disparities of Pediatric Brain Tumors
Email Principal Investigator

Xiao-Nan Li
CBTN Data
About this
Project
Brain tumors are the leading cause of cancer related death in children. While significant advances have been made in subgrouping tumors of the same diagnosis based on molecular findings, little is known about the differences of tumor biology and the clinical outcomes among racial/ethnic populations. Previous work involving the direct implantation of pediatric brain tumor tissues into the matching locations in the brains of SCID mice has highlighted remarkable differences of tumor take rate between children with different racial/ethnic groups. A recent CDC report also demonstrated an elevated rate of cancer diagnoses in white children (184.4/million) when compared with black children (133.3/million), Indigenous/Alaska native children (146.7/million) and Asian/pacific islander children (144.6/million). All of this combined information has led researchers to hypothesize that the overall responses to treatment may also be affected by the racial/ethnic differences in children with brain tumors. Identifying outcome differences and the underlying mechanisms will aid in improving therapeutics. This project will focus on understanding the survival disparity in pediatric brain tumors among children of different racial/ethnic groups. This work is made possible through access to comprehensive data from the Pediatric Brain Tumor Atlas.
Ask The
Scientists
What are the goals of this project?
Researchers seek to better understand the health and treatment outcome disparities of children with brain cancer across racial and ethnic groups.
What is the impact of this project?
Identifying outcome differences and the underlying mechanisms will aid in improving therapeutics.
Why is the CBTN request important to this project?
For this work to be comprehensive, researchers need access to the broad dataset on pediatric brain cancers provided by the Pediatric Brain Tumor Atlas.
Specimen Data
The Children's Brain Tumor Network contributed to this project by providing access to the Pediatric Brain Tumor Atlas.
Meet The
Team
related
Histologies
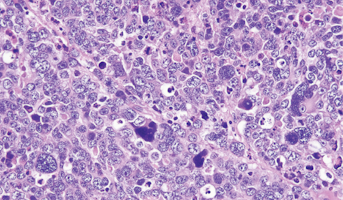
Medulloblastoma
Medulloblastomas comprises the vast majority of pediatric embryonal tumors and by definition arise in the posterior fossa, where they constitute approximately 40% of all posterior fossa tumors. Other forms of embryonal tumors each make up 2% or less of all childhood brain tumors.The clinical feature
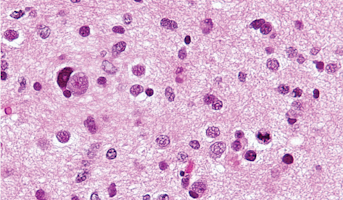
High-Grade Glioma
High-grade Gliomas (HGG) or astrocytomas in children nearly always result in a dismal prognosis. Although novel therapeutic approaches are currently in development, preclinical testing has been limited, due to a lack of pediatric-specific HGG preclinical models. These models are needed to help test
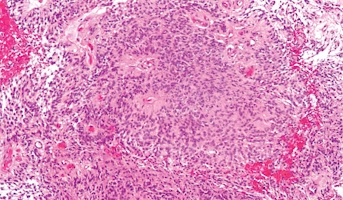
Ependymoma
Ependymomas arise from ependymal cells that line the ventricles and passageways in the brain and the center of the spinal cord. Ependymal cells produce cerebrospinal fluid (CSF). These tumors are classified as supratentorial or infratentorial. In children, most ependymomas are infratentorial tumors





