Carl Koschmann
Ann Arbor, MI USA
Michigan Medicine C.S. Mott Children’s Hospital

About
Assistant Professor
University of Michigan
Dr. Koschmann is a Pediatric Neuro-Oncologist in the Department of Pediatrics and a Principal Investigator of an independent translational Pediatric Neuro-Oncology laboratory at the Chad Carr Pediatric Brain Tumor Center at the University of Michigan. His work in the clinic and lab complements and drive each other, resulting in a clear goal to improve therapies for children and young adults with brain tumors. Dr. Koschmann’s R01-funded lab investigates the molecular mechanisms by which mutations in pediatric high-grade glioma (pHGG), including diffuse midline glioma (DMG) and DIPG promote tumor growth and affect response to therapy. His lab uses novel genetically engineered animal and in vitro/organoid models to uncover genetically driven therapeutic biomarkers in this patient population. Additionally, he serves as the Co-PI/Co-I for multiple early phase studies in pHGG/DMG for which his lab performs analysis of correlate tumor and CSF samples. Much of this work has been with CBTN- and PNOC-affiliated collaborations. Dr. Koschmann co-chairs the PNOC/CBTN DMG Working Group. He is leading efforts to coordinate the integration of pediatric brain tumor sequencing datasets from U of M (MiOncoseq) within CBTN. Finally, his lab developed the CNS-TAP precision medicine algorithm tool, which is being employed in PNOC008 currently, and for which integration with CBTN is underway.

Michigan Medicine C.S. Mott Children’s Hospital
scientific
Projects

Specimen
Ongoing
MET Alterations in DMGs
Recent work has pointed to dysregulation of a cellular process called the mesenchymal-epithelial transition (MET) as a driver for diffuse midline gliomas (DMGs). This project will further explore this dysregulation in an effort to identify new therapeutic targets for DMGs.
HGG, DIPG

Payal Jain

Specimen
Ongoing
Regional Response to ONC201 in Pediatric High-Grade Glioma
New targeted therapies are needed to address pediatric high grade gliomas with H3K27M mutations. The Children’s Brain Tumor Network will provide researchers with pHGG cell lines and data to pursue the development of therapeutics.
HGG, DIPG

Carl Koschmann
Specimen
Ongoing
Comparison of Fusion Calling Platforms in Pediatric DIPG and High‐grade Glioma
Targeted therapeutic options are limited for patients with diffuse intrinsic pontine glioma (DIPG). Researchers will perform state of the art analysis on data from the Pediatric Brain Tumor Atlas in an effort to identify new therapies for patients with DIPG.
DIPG

Carl Koschmann

Support
Data
Ongoing
MI-ONCOSEQ DMG Study
The University of Michigan established the Michigan Oncology Sequencing Center (MI-ONCOSEQ) to use high throughput DNA sequencing technologies to advance the goals of precision cancer medicine. An “integrative sequencing approach” carried out in a CLIA-certified laboratory is utilized to provide a c

Carl Koschmann
research
Interests
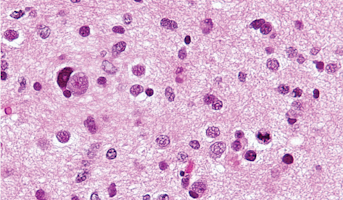
High-Grade Glioma
High-grade Gliomas (HGG) or astrocytomas in children nearly always result in a dismal prognosis. Although novel therapeutic approaches are currently in development, preclinical testing has been limited, due to a lack of pediatric-specific HGG preclinical models. These models are needed to help test
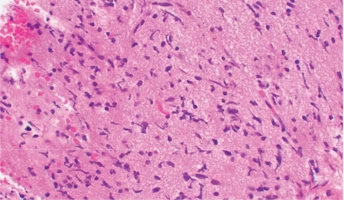
Diffuse Intrinsic Pontine Glioma
A presumptive diagnosis of DIPG based on classic imaging features, in the absence of a histologic diagnosis, has been routinely employed. Increasingly however, histologic confirmation is obtained for both entry into research studies and molecular characterization of the tumor.[5] New approaches with