Stewart Goldman

About
Division Head, Hematology, Oncology, Neuro-Oncology & Stem Cell Transplantation
Ann & Robert H. Lurie Children’s Hospital of Chicago
Stewart Goldman, MD is the head of the Division of Hematology, Oncology and Stem Cell Transplantation at the Ann & Robert H. Lurie Children's Hospital of Chicago and a professor in the Department of Pediatrics at Northwestern University Feinberg School of Medicine.
Goldman is the medical director and Gus Foundation Chair of Neuro-Oncology at Lurie Children's and focuses his clinical practice and research activities at Lurie Children's Falk Brain Tumor Center on pediatric brain tumors. He serves as the Chicago principal investigator for the Pediatric Brain Tumor Consortium as well as the Children's Oncology Group's Developmental Therapeutics Consortium site at Lurie Children's.
As director of the Clinical Trials Research Center at the Stanley Manne Children's Research Institute, Goldman is involved in developing and teaching new treatments for brain tumors. He has a special interest in developing new therapies for the treatment of brain stem gliomas and brain tumor survivorship issues.

Ann & Robert H. Lurie Children’s Hospital of Chicago
research
Interests
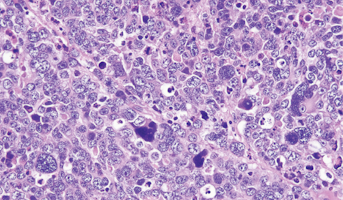
Medulloblastoma
Medulloblastomas comprises the vast majority of pediatric embryonal tumors and by definition arise in the posterior fossa, where they constitute approximately 40% of all posterior fossa tumors. Other forms of embryonal tumors each make up 2% or less of all childhood brain tumors.The clinical feature
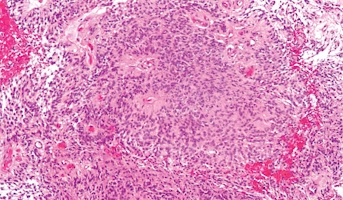
Ependymoma
Ependymomas arise from ependymal cells that line the ventricles and passageways in the brain and the center of the spinal cord. Ependymal cells produce cerebrospinal fluid (CSF). These tumors are classified as supratentorial or infratentorial. In children, most ependymomas are infratentorial tumors
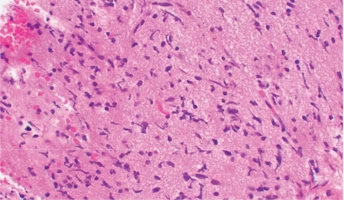
Diffuse Intrinsic Pontine Glioma
A presumptive diagnosis of DIPG based on classic imaging features, in the absence of a histologic diagnosis, has been routinely employed. Increasingly however, histologic confirmation is obtained for both entry into research studies and molecular characterization of the tumor.[5] New approaches with

