Comparison of CBTN Patient Data with Molecularly-Defined Stem Cell Models of Pediatric Brain Tumors
About this
Project
Preclinical models are a common way for researchers to study tumor types as well as test diagnostics and therapies. Researchers are currently developing various models of malignant pediatric tumors such as medulloblastoma, malignant glioma, diffuse intrinsic pontine gliomas (DIPG) and choroid plexus carcinomas. The focus of this research is on the signaling pathways of MYC and MYCN cancer genes. These pathways are commonly dysregulated in childhood brain tumors and a deeper understanding of this dysregulation could lead to more accurate diagnoses and new therapeutics. Researchers will compare patient-derived gene expression profiles housed in the Pediatric Brain Tumor Atlas to data generated from models. This will allow researchers to validate that their newly developed models are accurate and relevant to medical professionals.
Ask The
Scientists
What are the goals of this project?
Researchers seek to validate the accuracy of newly developed preclinical models for malignant brain tumors.
What is the impact of this project?
This research will allow researchers to make sure that newly developed models will be accurate and relevant. Robust preclinical models are important for understanding drug interactions in pediatric brain cancer patients and to support the discovery of new therapeutics.
Why is the CBTN request important to this project?
To validate their newly developed models, researchers will compare preclinical model derived data to comprehensive pediatric cancer data available through the Pediatric Brain Tumor Atlas.
Specimen Data
The Children's Brain Tumor Network contributed to this project by providing access to the Pediatric Brain Tumor Atlas.
Meet The
Team
Institutions

Primary
Children’s National Hospital
Joined onEach year, the Brain Tumor Institute at Children’s National evaluates more than 100 new patients with brain tumors, and is recognized as a world leader in childhood brain tumor care and research. Children’s National has pioneered novel pediatric brain tumor therapies, including new molecularly-targe


Uppsala University
related
Histologies
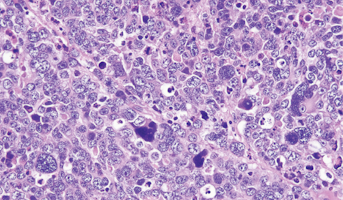
Medulloblastoma
Medulloblastomas comprises the vast majority of pediatric embryonal tumors and by definition arise in the posterior fossa, where they constitute approximately 40% of all posterior fossa tumors. Other forms of embryonal tumors each make up 2% or less of all childhood brain tumors.The clinical feature
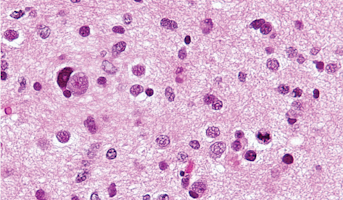
High-Grade Glioma
High-grade Gliomas (HGG) or astrocytomas in children nearly always result in a dismal prognosis. Although novel therapeutic approaches are currently in development, preclinical testing has been limited, due to a lack of pediatric-specific HGG preclinical models. These models are needed to help test
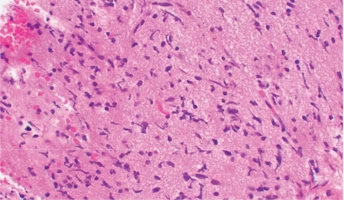
Diffuse Intrinsic Pontine Glioma
A presumptive diagnosis of DIPG based on classic imaging features, in the absence of a histologic diagnosis, has been routinely employed. Increasingly however, histologic confirmation is obtained for both entry into research studies and molecular characterization of the tumor.[5] New approaches with
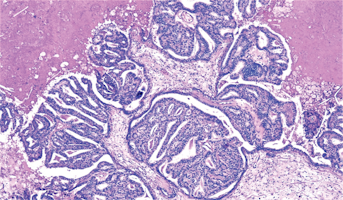
Choroid Plexus Carcinoma
Choroid plexus tumors (Grade III) occur in both children and adults, but are more common in children in the first year of life. Choroid plexus tumors occur slightly more often in females than males.The cause of most choroid plexus tumors is not known. Genetic changes have been linked to the formatio



