Sabine Mueller
San Francisco, CA USA
UCSF Benioff Children's Hospital

About
Professor of Clinical Neurology
UCSF Benioff Children's Hospital
Dr. Sabine Mueller is a pediatric neuro-oncologist who specializes in caring for children with brain tumors and related genetic syndromes. Before completing medical school, she worked as a scientist, director of genomics and project leader for a brain tumor program at AGY Therapeutics, a biotechnology company in South San Francisco.
In her research, Mueller studies treatments for children with brain tumors, looking especially at improving long-term cognitive outcomes.
Mueller earned her medical degree at the Universität Hamburg Faculty of Medicine and earned a doctorate in biochemistry and molecular biology in collaboration with AGY. After a residency in pediatrics at Massachusetts General Hospital, she completed a fellowship in pediatric oncology at UCSF.

UCSF Benioff Children's Hospital
scientific
Projects

Specimen
Ongoing
Oncolytic Virus to Potentiate Immune-checkpoint Blockade in Immunologically Cold Pediatric Brain Tumors
The use of an oncolytic virus refers to the use of a virus to stimulate immune response in a tumor. Researchers will utilize carefully catalogued samples provided by the Children’s Brain Tumor Network to further explore the use of oncolytic viruses in the treatment of pediatric brain cancers.
Medulloblastoma

Aaron Diaz

Data
Planning
Precision Imaging of Pediatric High-grade Gliomas with Quantitative Diffusion Weighted Imaging and Texture Analysis to Identify Imaging Biomarkers That Predict Tumor Genetics and Patient Outcomes
The recently characterized molecular marker, histone H3 K27M, could prove important to the treatment of pediatric gliomas. Researchers will interrogate data from the Pediatric Brain Tumor Atlas in order to better understand this new class of malignant gliomas.
HGG, DIPG

Mariam Aboian
Data
Ongoing
Integrative Analysis of Childhood Cancers
Integrative research is needed to advance the treatment options for pediatric cancers. Researchers will analyze data provided through the Pediatric Brain Tumor Atlas in an effort to identify new opportunities in the treatment of pediatric cancers.
All Brain Tumor Types

Charlie Vaske

Data
Ongoing
PNOC and SJCRH Collaborative DIPG Radiogenomic Investigation
Tumor classification through imaging is an important part of pediatric cancer diagnosis and treatment. Researchers will investigate tumor imagery and genomic data provided by the Children’s Brain Tumor Network in an effort to advance the accuracy of tumor classification.
DIPG
Data
Ongoing
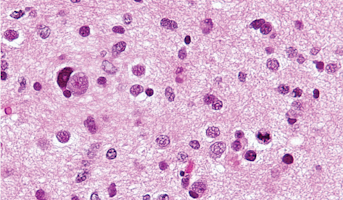
Using histopathology to discover genetic alterations in pediatric brain tumors
In depth understanding of the molecular make up of brain tumors is critical to inform therapy decision making. Often tumor tissue is limited for this type of analysis and it will be very beneficial to derive detail molecular information from basic pathology slides. Herein we aim to use machine learning to develop such program that will allow us to predict the molecular make up based on analysis of standard pathology slides. Funding for the project was provided by Ian’s Friends Foundation.
All Brain Tumor Types

Sabine Mueller
research
Interests
High-Grade Glioma
High-grade Gliomas (HGG) or astrocytomas in children nearly always result in a dismal prognosis. Although novel therapeutic approaches are currently in development, preclinical testing has been limited, due to a lack of pediatric-specific HGG preclinical models. These models are needed to help test
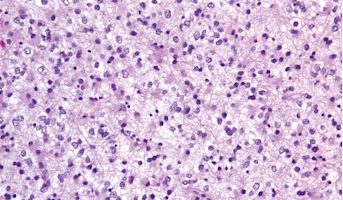
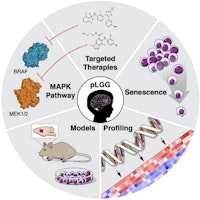
Low-Grade Glioma
Low-Grade Gliomas also called astrocytomas are the most common cancer of the central nervous system in children. They represent a heterogeneous group of tumors that can be discovered anywhere within the brain or spinal cord. Although surgical resection may be curative, up to 20% of children still su
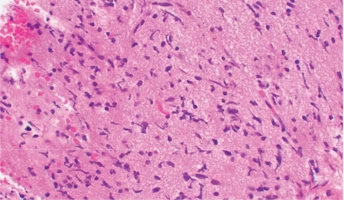
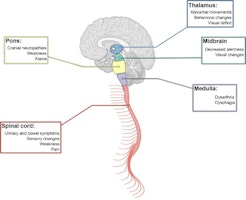
Diffuse Intrinsic Pontine Glioma
A presumptive diagnosis of DIPG based on classic imaging features, in the absence of a histologic diagnosis, has been routinely employed. Increasingly however, histologic confirmation is obtained for both entry into research studies and molecular characterization of the tumor.[5] New approaches with